Imagine waking up and finding that the center of your vision has a blurry spot or a dark hole. You can still see the edges of the room and walk around without bumping into furniture, but you can't read the morning news or recognize your spouse's face across the table. This is the reality for millions of people living with Age-Related Macular Degeneration is a progressive eye disease that causes the breakdown of the macula, the central part of the retina responsible for sharp, detailed vision. While it sounds frightening, we now have medical breakthroughs that can stop the decline and, in some cases, actually bring vision back.
Key Takeaways for Your Vision Health
- AMD targets your central vision, while peripheral vision usually stays intact.
- Dry AMD is more common, but Wet AMD causes the most severe, rapid vision loss.
- Anti-VEGF injections are the gold standard for treating the wet form of the disease.
- Early detection through annual exams and home monitoring is critical for saving sight.
- Lifestyle choices, especially quitting smoking, can significantly lower your risk.
What Exactly is Macular Degeneration?
To understand this condition, you first have to understand the Macula. This tiny area in the center of your Retina is packed with cone photoreceptors. These cells are the "high-definition" part of your eye; they handle color perception and the fine details you need for reading or driving. When the macula degenerates, you lose that central focus.
This isn't just a random occurrence of aging. It's a complex process where oxidative stress damages the outer retina. Over time, cellular debris builds up, and the eye's immune system can actually trigger an inflammatory response that damages healthy tissue. Because this happens slowly, many people don't notice it until a significant amount of vision is already gone.
Dry vs. Wet AMD: Knowing the Difference
Not all macular degeneration is the same. Doctors categorize it into two main types based on how the retina breaks down. While one is a slow fade, the other is a medical emergency.
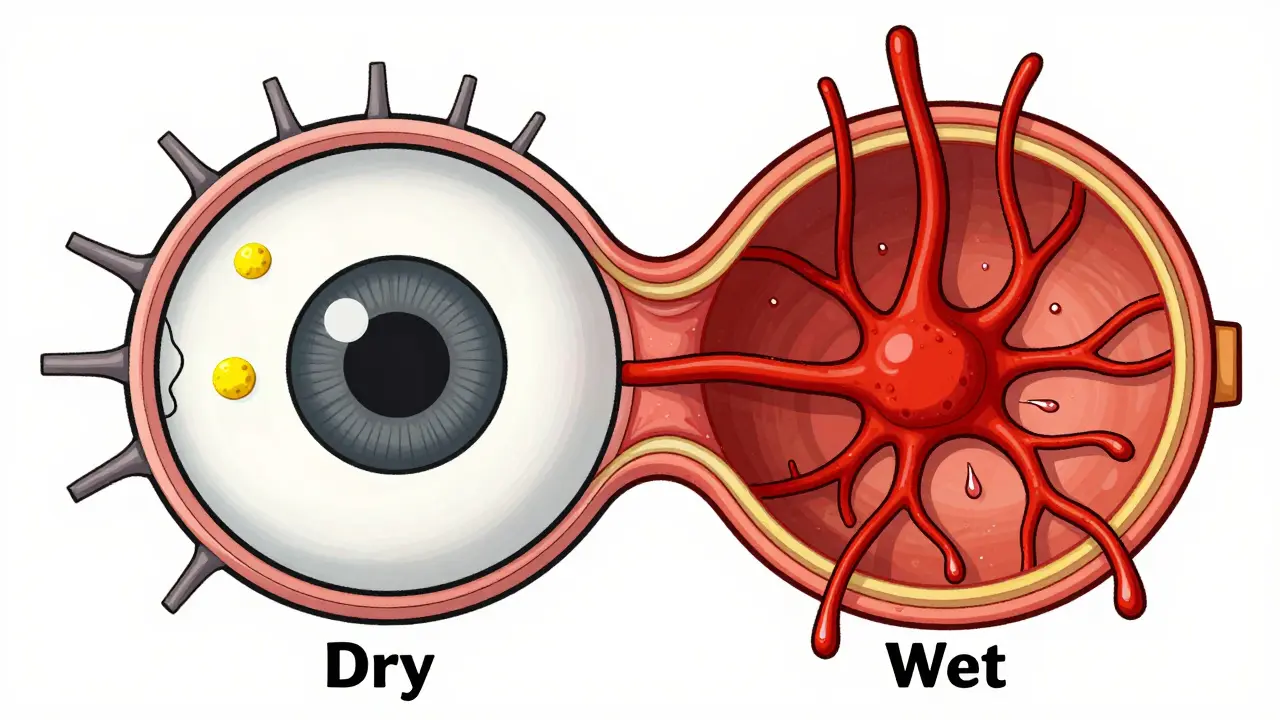
Dry AMD is the most common version, accounting for about 90% of cases. It happens when small yellow deposits called Drusen build up under the retina. These deposits cause the retinal tissue to thin and wither. It's a gradual process, and while it's frustrating, it usually moves slowly over years.
Then there is Wet AMD. This version is much more aggressive. It occurs when abnormal blood vessels start growing underneath the macula. These vessels are "leaky," meaning they spill blood and fluid into the retina. This causes rapid swelling and scarring. Although it only affects 10-15% of patients, it's responsible for the vast majority of severe vision loss. The scary part? Dry AMD can turn into Wet AMD at any time.
| Feature | Dry AMD (Non-Neovascular) | Wet AMD (Neovascular) |
|---|---|---|
| Prevalence | ~90% of cases | ~10-15% of cases |
| Main Cause | Thinning retina and Drusen buildup | Leaking abnormal blood vessels |
| Progression Speed | Slow, gradual decline | Rapid, can happen in months |
| Impact on Vision | Gradual loss of detail/contrast | Severe central blind spots (scotomas) |
| Primary Treatment | AREDS2 supplements (intermediate) | Anti-VEGF injections |
Who is at Risk?
Age is the most obvious factor-it's in the name, after all. If you're over 75, the odds of having some form of AMD jump significantly. However, age isn't the only piece of the puzzle. Genetics play a huge role; if your parents or siblings had it, your own risk could be 3 to 6 times higher.
But here is the good news: there are things you can actually control. Smoking is the single biggest modifiable risk factor. If you smoke, you're nearly four times more likely to develop the disease than someone who never has. Other health issues like high blood pressure, high cholesterol, and obesity (specifically a BMI over 30) also push the risk higher. Essentially, anything that damages your blood vessels or increases inflammation in the body can make your eyes more vulnerable.
Anti-VEGF Therapy: The Modern Solution for Wet AMD
For decades, we didn't have a great way to stop Wet AMD once it started. Then came Anti-VEGF Therapy. To understand how it works, you need to know about Vascular Endothelial Growth Factor (VEGF), a protein in the body that tells the system to grow new blood vessels. In a healthy eye, this is fine. In a diseased eye, too much VEGF causes those "leaky" vessels to sprout in the wrong place.
Anti-VEGF medications are antibodies that bind to this protein and neutralize it. By blocking VEGF, the drugs stop the growth of new abnormal vessels and dry up the fluid already leaking into the retina. This prevents further scarring and can actually restore some of the lost vision.
The catch? These drugs have to be injected directly into the eye (intravitreal injection) because they can't reach the retina through a pill or a standard vein injection. For many, the thought of a needle in the eye is terrifying. But the results are often life-changing. One patient reported their vision stabilizing at 20/40 after a series of injections, moving up from a nearly blind 20/200. That's the difference between needing a caregiver and being able to drive yourself to the store.
The Practical Side of Living with AMD
Managing this condition requires a partnership between you and your ophthalmologist. If you have dry AMD, you might be prescribed the AREDS2 formula-a specific blend of antioxidants and minerals. For people with intermediate dry AMD, this supplement can reduce the risk of progressing to the advanced stage by about 25%.
If you're in the "wait and watch" phase, you should use an Amsler Grid. This is a simple grid of straight lines. You look at the center dot and check if any of the lines look wavy or distorted. If they do, it's a red flag that your dry AMD may have turned "wet," and you need to get to a clinic immediately.
For those on Anti-VEGF treatment, the schedule is demanding. Usually, it starts with monthly injections for three months, followed by "as-needed" doses based on scans called Optical Coherence Tomography (OCT). These scans allow doctors to see the layers of the retina in microscopic detail to decide if another shot is necessary. Missing these appointments is dangerous; patients who miss more than a quarter of their injections often see a 30% drop in vision.

The Future: Moving Beyond Monthly Shots
The biggest complaint from patients isn't the needle-it's the commute. Frequent clinic visits are a massive burden. This is why the industry is moving toward longer-lasting options. We now have port delivery systems, like the Susvimo implant, which can provide a continuous stream of medication for up to six months, eliminating the need for monthly trips.
Even more exciting is the move toward gene therapy. Scientists are looking at the complement pathway genes, which are responsible for much of the genetic risk of AMD. By fixing the genetic "glitch" at the source, we might one day move from managing the disease with injections to curing it entirely. In the meantime, new "bispecific" antibodies are hitting the market that target not just VEGF, but other proteins like angiopoietin-2, offering better stability for more people.
Can you fully cure macular degeneration?
Currently, there is no cure that completely reverses AMD. However, Anti-VEGF therapies can stop the progression of wet AMD and can sometimes improve vision by reducing swelling and leakage in the retina. For dry AMD, supplements like AREDS2 can slow the decline.
Does AMD cause total blindness?
AMD causes loss of central vision, but it typically does not cause total blindness. Your peripheral (side) vision remains intact, meaning you can still see objects around you, though you won't be able to see the fine details of a face or a page of text.
How often do I need Anti-VEGF injections?
The schedule varies by patient. A common starting point is once a month for the first three months. After that, your doctor will use OCT scans to determine if you need shots every 4 to 8 weeks, or if you can move to an "as-needed" schedule.
What are the warning signs that Dry AMD has turned Wet?
The most common sign is the appearance of wavy or distorted lines (metamorphopsia). If straight edges-like a door frame or a line of text-suddenly look bent, or if a dark spot appears in the center of your vision, contact your ophthalmologist immediately.
Is the Amsler Grid actually effective?
Yes, it's a highly effective tool for home monitoring. Evidence suggests that about 40% of patients detect changes in their vision using the grid before their scheduled clinical visit, allowing for faster treatment and better vision preservation.
Next Steps for Your Eye Care
If you're over 65, the best thing you can do is schedule a comprehensive eye exam. Don't wait for symptoms to appear, because by then, the damage has already started. If you already have a diagnosis, keep a strict calendar for your injections and use your Amsler grid daily.
For those struggling with the side effects or the frequency of treatment, ask your eye surgeon about the latest port delivery systems or bispecific antibodies. The technology is moving fast, and you shouldn't have to settle for a treatment plan that disrupts your entire life.






Comments
Just a heads up for anyone starting the Anti-VEGF shots, the numbing drops help a ton but don't be surprised if you see a few floaters for a couple of days after the procedure. It's super common and usually clears up on its own, but definitely let your doctor know if you see a sudden increase in flashes of light.
The simplistic presentation of the complement pathway is quite pedestrian. One would hope for a more rigorous exploration of the genetic polymorphisms involved, rather than this superficial overview that caters to the lowest common denominator of medical literacy.
It is truly heartening to see the progress in medical science, and for anyone out there feeling overwhelmed by the prospect of these injections, just remember that you are not alone in this journey and there are so many supportive communities and wonderful healthcare professionals who are dedicated to helping you maintain your independence and quality of life through every single step of the process.
People just don't take care of their bodies. If you eat junk and smoke, you can't act surprised when your eyes fail you. It's all about energy and balance, which most people totally ignore until it's too late.
glad these new implants are coming out 😌 saves so much driving time lol
The efficacy of bispecific antibodies targeting both VEGF and angiopoietin-2 suggests a synergistic effect in stabilizing the vascular endothelium. I suspect the reduction in extravasation is more pronounced in patients with chronic edema.
Quit smoking. It's not rocket science. If you can't do that one thing for your health, you're basically asking for these blind spots.
Oh please! As if an Amsler grid is some magical shield against blindness! The sheer drama of telling people to run to a clinic the moment a line looks slightly bent is absolutely absurd and just creates unnecessary panic for everyone involved!
The tragedy of the human condition is that we spend our final years fighting for the right to see the faces of those we love, yet we spent our youth ignoring the very habits that steal that sight away. It is a moral failing of the modern age that we prioritize convenience over the sanctity of our biological vessels, and now we rely on synthetic antibodies to patch up the holes we tore in our own wellbeing. How utterly bleak is the reality where a needle in the eye is our only salvation from a darkness we invited in through sheer negligence and a lack of spiritual discipline. We are merely ghosts in a machine, desperately trying to calibrate our lenses while the clock runs out on our existence, and the irony is that we think a 'port delivery system' is the peak of human achievement when we cannot even master the art of living simply. I find it almost comedic, in a dark sort of way, that we celebrate the ability to drive to a store while our souls are blind to the decay of our own nature. It is a farce, a complete and utter farce, to believe that medical intervention can replace the void left by a life spent in imbalance and toxins. Truly, we are witnessing the decline of the human spirit manifested as a blur in the center of the retina, a poetic reflection of our own internal blindness. We chase these 'breakthroughs' like dogs chasing cars, never realizing that the road we are on leads directly to the void regardless of how sharp our vision is. What a miserable state of affairs!
The idea of gene therapy is just beautiful 🌟 it shows how we can collaborate with nature to fix things from the root! Love seeing the hope this brings to so many people! ❤️
It is simply common sense to follow a medical schedule. People who miss their shots are just lazy.
I agree that early detection is the most important part of this. My uncle had this and catching it early really changed his outcome.
It makes you think about how much we take for granted until it's gone. Vision is so tied to how we experience the world, and the fact that we can now manage this is pretty wild.
The information provided is very clear.
While I appreciate the effort to explain these medical procedures, I find it absolutely unacceptable that some people try to dismiss the struggle of those with genetic predispositions as 'laziness' or 'poor choices' when the biological reality is far more complex than a simple lifestyle change, and we should be fostering a spirit of global cooperation and understanding rather than attacking the vulnerable who are simply trying to navigate a devastating disease with the limited tools available to them in their respective corners of the world.